Coronavirus Tests. Why Can't We Do More of Them?
 To do coronavirus tests, you need advanced equipment and trained staff. Source: Central Clinical Hospital of the Medical University of Lodz
To do coronavirus tests, you need advanced equipment and trained staff. Source: Central Clinical Hospital of the Medical University of Lodz
Advanced equipment, trained staff and access to biological material are needed to do coronavirus tests. But only certain facilities have them and there are also a limited number of people who know how to use this equipment.
In addition, the amount of financial resources for testing, the availability of testing equipment, the capacity of laboratories need to also be factored in as do the logistics related to the collection of test material, the number of patients and data reporting system.
Geneticist and laboratory diagnostician, Professor Maciej Borowiec from the Medical University of Łodz talks about how coronavirus tests work and how many can be carried out in Poland.
“It's an entire system that needs to work. If the system works efficiently, we can see fluidity in sample processing.” he says.
MAINLY RESEARCHERS USED MACHINES FOR TESTING
RT-PCR (polymerase chain reaction) technology is mainly used in Poland to perform coronavirus tests. However, only some facilities have RT-PCR machines. “These are mainly clinical hospitals operating at academic centres and hospitals that deal with difficult diseases. This equipment is also available in natural science universities and some research institutes. In short, institutions around which numerous groups of scientists are gathered,” explains Professor Borowiec.
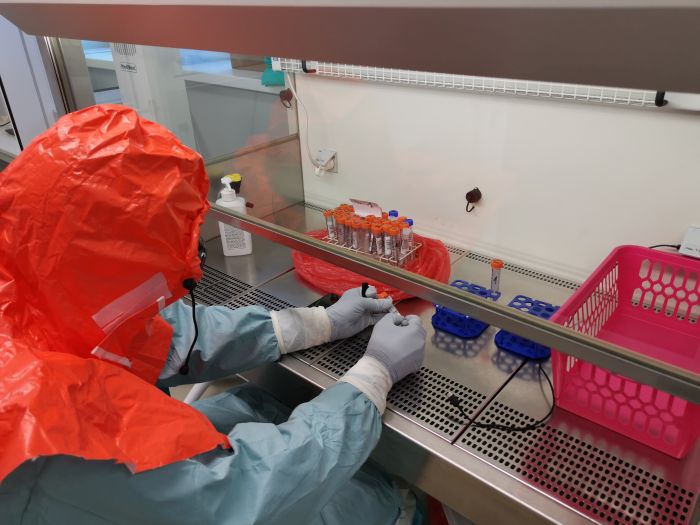
To do coronavirus tests, you need advanced equipment and trained staff. Source: Central Clinical Hospital of the Medical University of Lodz
“The use of these devices is very broad,” he emphasizes, adding that RT-PCR machines have so far been used in scientific research or diagnosis of influenza, CMV, HPV and many other pathogens, and in the diagnosis of genetic causes of diseases. Scientific research was also conducted on them, for example analysis of the expression of genes associated with specific diseases.
QUALIFIED STAFF
“In addition to equipment, we must have specific human resources,” he says, explaining that expert knowledge is needed to work in a laboratory. RT-PCR has been used by geneticists, molecular biologists and biotechnologists. Now they are working on SARS-CoV-2 tests under the supervision of laboratory diagnosticians, which results from legal requirements. “Working in a laboratory where you work on COVID-19 is not nice, easy and pleasant work. We need protective clothing, aprons, leg protectors, protective suits. We work in conditions that are far from comfortable.”
PATH OF THE SAMPLE
In a coronavirus test, the sample is taken using a nasopharyngeal swab. Usually, hospital employees, medical staff and emergency services do this. The sample, properly secured and marked, goes to crisis management systems, for example provincial sanitary services or provincial emergency medical station. The material is catalogued and then distributed to appropriate laboratories. In Łódź, where Borowiec works, there are three such laboratories.
After the sample is delivered to the laboratory, the biological material is inactivated (viruses must be neutralized, for example by high temperature treatment). Then the genetic material of the virus is isolated. The Real Time PCR reaction allows them to analyse the presence of virus RNA in the sample to detect RNA fragments typical for SARS-Cov-2 (in the test used in Professor Maciej Borowiec's laboratory it is the ORF1ab fragment and the N fragment of the virus end). One of the available genetic tests is used for this. These fragments are appropriately marked in the test so that they glow when illuminated by laser light. Professor Borowiec says that in his laboratory, the analysis of 90 samples takes about 5-6 hours.
WHEN DOES THE GENETIC METHOD WORK?
This method detects the presence of virus RNA in the patient's mucosa. This means that this is the moment when the virus already multiplies in the body.
“The tests detect the virus at different levels of sensitivity; the above test detects the virus at the level of a minimum of 200 copies in the genetic material. This is a very sensitive method,” says Borowiec.
He notes that the test is unlikely to work, for example, on the same day when the subject had contact with an infected person. To be detected, the virus must have a chance to multiply in the body.
SEPARATE TEST - ANTIBODY DETECTION
A genetic test is based on the identification of the viral RNA genetic material. Immunoassay is a separate matter. It is based on the identification of antibodies that the body produces against the coronavirus protein. Instead of detecting the presence of the virus, the test detects the substances that show that the body is defending itself against the virus.
These tests are already carried out in Polish hospitals quite often. But Professor Borowiec warns that their results can be misleading. During the first few days of infection, the body can already spread the virus, but the immune system still has not managed to produce a response to the pathogen. “If we do the test too soon, we may mistakenly conclude that the person is healthy. The patient will be released and infect others. And after a few days we will have more infected people,” says Borowiec. He explains that the RNA test performed at that point would confirm the infection.
WHAT ABOUT CONVALESCENTS?
He also says that the antibody test can detect whether a person has already had the infection (for example an asymptomatic one), as “there should be antibodies in the blood, while the PCR test will no longer identify viral RNA.”
But he says that then a problem arises. “The patient has an immune response, but we did not catch them during the inflamed situation when the patient was most contagious. Should we keep them in quarantine? Should we diagnose their family and the people they have been in contact with? And when exactly was that person actually contagious? When we start thinking about it, it may be logistically confusing, because it turns out that everyone should be quarantined for some time.”
TEST ACCURACY? TIME WILL TELL
Asked about the accuracy of coronavirus tests (the percentage of false positive or false negative results), Professor Maciej Borowiec says that it is still unknown. This can only be determined after the epidemic ends or its intensity decreases. In other words, when we can analyse the data from most centres testing biological material for coronavirus.
PAP - Science in Poland, Ludwika Tomala
lt/ zan/ kap/
tr. R
Przed dodaniem komentarza prosimy o zapoznanie z Regulaminem forum serwisu Nauka w Polsce.